From Cath Lab to Follow-Up Closing Data Gaps in Cardiology Workflows
Cardiology workflow optimization begins with understanding where care transitions break. In most cardiology programs, the workflow doesn’t fail inside the cath lab or clinic. It fails in the space between them, where communication and processes can break down. Data gaps in healthcare show up at every handoff; this includes diagnostics, intervention, recovery, and follow-up. When teams delay or share incomplete information, they lose visibility. This can cause patients to fall through the cracks.
The most critical failures in cardiology workflows don’t occur during procedures when they occur during transitions between diagnostics, intervention, discharge, and follow-up.
For a deeper look at how analytics strengthens modern cardiology programs, explore our guide on The Role of Data Analytics in Modern Cardiology Care Delivery.
Modern cardiology care delivery spans multiple settings and teams. Each transition brings risks. These include data loss, communication delays, and missed chances for help. Closing these gaps improves outcomes. It strengthens care coordination and reduces operational strain. Best of all, it does this without adding new administrative burdens.
Understanding the End-to-End Cardiology Care Workflow
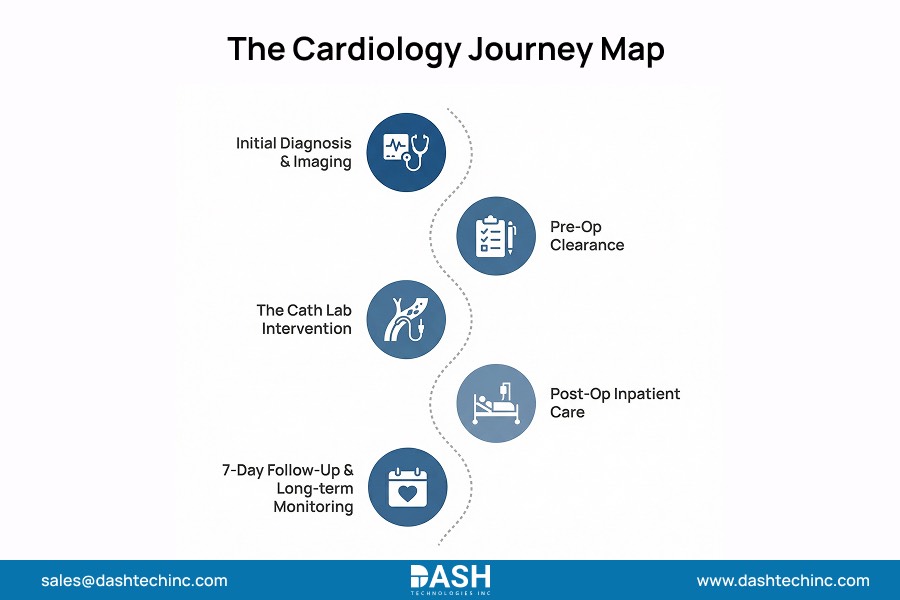
Cardiology care workflows cover a wide range. Each step produces important clinical data. Data must move seamlessly across systems to enable cardiology workflow optimization.
- Pre-Procedure Evaluation
The end-to-end cardiology workflow begins with the aggregation of history, physicals, and diagnostic imaging (ECG, Echo, Stress tests) to determine the necessity of intervention. - Cath Lab and Intervention
Procedural details and hemodynamics are key. Device info, complications, and post-procedure orders are the “source of truth.” They determine what happens next in healthcare workflow analytics. - Inpatient Recovery and Discharge
Vitals, complications, meds reconciliation, and discharge instructions bridge inpatient to outpatient. Missing data here leads to redundant work or gaps. - Outpatient Follow-Up and Monitoring
Post-discharge visits, remote monitoring, & medication titration help track long-term outcomes. This continuity helps find problems early. This includes stent thrombosis and heart failure decompensation.
Where Cardiology Data Gaps Commonly Occur in Workflows
Despite advanced technology, fragmented cardiology workflows remain common. Breakdowns typically occur at transition points, highlighting the critical need for cardiology workflow optimization.
Between Diagnostics and the Cath Lab
- Imaging and test results stored in separate systems
- Referral information missing or incomplete
- Scheduling delays due to limited data visibility
During Post-Procedure Transitions
- Procedural notes not immediately available to recovery teams
- Medication updates delayed or unclear
- Limited visibility into discharge planning
Between Discharge and Follow-Up Care
- Missed follow-up appointments
- Lack of communication with primary care providers
- Limited tracking of patient adherence and outcomes
These breakdowns are predictable and preventable.
The Clinical and Operational Impact of Cardiology Data Gaps
Gaps don’t just affect patients; they create operational inefficiencies cardiology-wide. When cardiology care coordination relies on incomplete handoffs, the result is both clinical risk and operational drag.
Common impacts include:
- Delayed follow-ups: Patients can slip through the cracks. This often happens when a follow-up step isn’t scheduled or confirmed.
- Redundant tests: When lab results aren’t available during a care transition, it’s easier just to reorder the test. This wastes time and resources.
- Missed risk signals: Post-procedure warnings, abnormal lab results, or symptom patterns aren’t escalated in a timely manner.
- Increased clinician workload: Teams spend time on “detective work”—calls, chart hunting, and re-documenting information.
This is where healthcare workflow analytics becomes essential: you can’t fix what you can’t see, and you can’t sustain improvements if the burden stays manual.
.jpg)
Comments
Post a Comment